Published: 04/16/2012 Updated: 05/20/2021
No other infectious disease raises as many questions as tick-borne borreliosis. The reasons for this are the diversity of the clinical picture of the disease, different opinions of specialists regarding the diagnosis and treatment of this disease, and low awareness of the population about this disease. In this review, we will try to provide the most objective information about this disease, as far as possible at present. This review is based mainly on data from European experts (EUCALB).
What is borreliosis (Lyme disease)
Lyme disease (tick-borne systemic borreliosis, Lyme borreliosis) is a transmissible, natural focal disease characterized by damage to the skin, joints, nervous system, heart, often taking a chronic, relapsing course. Among infectious diseases transmitted by ticks, Lyme disease (LD) is the most common. The name of the disease comes from the name of the small town of Old Lyme in Connecticut (USA), where in the mid-1970s a number of cases of arthritis after tick bites were described. In Europe, Borrelia infection had already been known for a long time under various names (erythema migrans, Bannwart syndrome), but the pathogen was isolated only in 1982.
Lyme disease - symptoms and treatment
The incubation period in various sources ranges from 1 to 50 days (in practice, a period of 1-30 days should be adhered to).
Disease syndromes:
- general infectious intoxication;
- erythema (redness of the skin);
- arthritis;
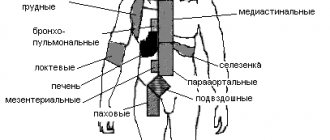
- regional lymphadenopathy (enlarged lymph nodes);
- damage to the nervous system;
- damage to the cardiovascular system;
- hepatolienal (enlarged liver and spleen).
The periods of development of the disease are quite conditional, mostly limited only by time frames:
- early (localized and disseminated stages);
- late;
- residual.
Localized early stage
It begins acutely or subacutely with low fever (low-grade body temperature - 37.1-38°C), headache, weakness, discomfort in muscles and joints. Nausea and vomiting are rare. Catarrh (inflammation) of the upper respiratory tract occurs very rarely, sometimes regional lymphadenopathy and hepatolienal syndrome occur.
The most striking sign of this phase of the disease (however, not always!) is the appearance of migrating annular erythema on the surface of the skin (a pathognomonic sign of the disease). First, at the site of localization of the tick bite, a primary affect occurs (redness of 2-4 mm of a reddish color), then a spot or papule of intense pink-red color appears, spreading in all directions many centimeters in diameter over the course of several days. The edges of the spot become clearly defined, bright red, slightly rising above the level of unchanged skin. More often, in the center, the spot slowly fades, becomes cyanotic (turns blue), and the formation takes on the characteristic appearance of an oval or round ring-shaped erythema.
At the site of erythema localization, itching and mild pain cannot be ruled out. In the absence of antibiotic therapy, erythema is visualized within several days; in their absence, it can last up to two months or more. The result is weak short-term pigmentation and peeling. In some patients, several erythemas of smaller diameter appear (usually in a later period).
Early disseminated stage
This stage begins at 4-6 weeks of illness (in the absence of preventive and therapeutic therapy during the previous period). During this period, the previous symptoms (syndrome of general infectious intoxication, fever and erythema) fade away. Neurological disorders are detected:
- mild encephalitis,
- mononeuropathy,
- serous meningitis,
- encephalomyelitis with radiculoneuritic reactions,
- lymphocytic meningoradiculoneuritis, characterized by pain at the site of the bite, severe radicular pain with impaired sensitivity and motor function of the cervical and thoracic spinal cord - the so-called Bannworth syndrome, including the triad: radicular pain, peripheral paresis (usually the facial and abducens nerves) and lymphocytic cellular reaction with cell content from 10 to 1200 per mm3) when performing a lumbar puncture.
Possible damage to the cardiovascular system - cardialgia, palpitations, increased blood pressure, myocarditis, AV blockade (impaired transmission of nerve impulses in the conduction system of the heart).
Sometimes there are skin lesions (urticarial and other rashes). Borreliosis lymphocytoma (benign lymphadenosis of the skin) may be observed - a bluish-red skin infiltrate with lymphoreticular proliferation, mainly located on the earlobe or nipple of the breast. Rarely, eye lesions occur in the form of conjunctivitis, choroiditis, and iritis.
Mild hepatitis and kidney dysfunction cannot be ruled out.
Joint lesions in the form of reactive arthritis (mainly large joints) in the form of pain and limitation of mobility, without external changes, lasting from a week to three months. Without treatment, Lyme disease becomes chronic.
Late period of Lymeborreliosis
Begins 1-3 months after the early one or more. Reminiscent of asthenoneurotic syndrome: weakness, increased fatigue, decreased mnestic functions (memory and intelligence), cranialgia (headache), sleep disturbances, increased nervous excitability or depression, muscle pain. Inherent damage to the musculoskeletal system (initially, migrating arthralgias without obvious inflammation), then benign recurring arthritis with inflammation and a slow transition to a chronic progressive course (with irreversible changes in the structure of the joints - marginal and cortical lesions (erosions), osteophytes, sclerosis). There may be dermatitis, scleroderma, paraparesis, neuritis, memory disorders. A characteristic lesion is atrophic acrodermatitis - the gradual appearance of cyanotic-red spots on the extensor surfaces of the extremities, nodules, infiltrates, and sometimes the skin takes on the appearance of “tissue paper.”
Reinfection has been described - “fresh” creeping erythema, congenital Lyme borreliosis.
Borreliosis in pregnant women
Infection of a woman during pregnancy (and before it in the absence of treatment) increases the risk of fetal death and miscarriage. Intrauterine damage to the fetus with the development of encephalitis and carditis is possible, but the magnitude of the risk of this remains unclear.
Differences between borreliosis in children
Lyme disease in children most often develops between the ages of 3 and 10 years. In this case, erythema migrans (redness of the skin) often appears, located in the upper half of the body. Intoxication is usually stronger than in adults. Lymph nodes near the site of the tick bite may become enlarged. Without treatment, up to 20% of Lyme disease cases become chronic.
Differential diagnosis:
- in the first phase - febrile conditions with exanthema, tick-borne encephalitis, erysipelas, erysipeloid, cellulitis;
- in the second stage - serous meningitis of another etiology, tick-borne encephalitis, rheumatic carditis;
- in the third stage - rheumatism and similar diseases, rheumatoid arthritis, Reiter's disease.[3][6]
Differences from tick-borne encephalitis
With tick-borne encephalitis, there is severe fever, cerebral and neurological symptoms, with borreliosis - damage to the skin, joints and heart.
Pathogens
The causative agents of Lyme disease are several species of human pathogenic borrelia - Borrelia burgdorferi, Borrelia garinii and Borrelia afzelii. Borrelia are microaerophiles and, like other gram-negative spirochetes, are extremely demanding on cultivation conditions. Infections caused by Borrelia burgdorferi most often present with arthritis (especially in North America, where it is the only causative agent of borreliosis), while B. garinii is more likely to cause neurological disorders and B. afzelii is more likely to cause chronic skin diseases. All three pathogens cause erythema migrans.
Epidemiology
The natural hosts of Borrelia in nature are wild animals (rodents, birds, deer), which feed ticks of the genus Ixodes - carriers of Borrelia. During blood sucking, borrelia enter the tick's intestines, where they multiply and are excreted in feces. Despite the high level of infection of ticks, the possibility of infection through a bite is not always realized, because borrelia are contained in the salivary glands in small quantities or are absent altogether.
In natural foci, the circulation of the pathogen occurs as follows: ticks → wild animals → ticks. It is possible that domestic animals - goats, sheep, cows - may be involved in the epidemiological chain. The likelihood of other carriers of Borrelia, such as horse flies, is being studied. A person becomes infected with Lyme disease in natural foci. Natural foci of Lyme disease are found mainly in forest landscapes of the temperate climate zone. In recent years, it has been established that the area of distribution of tick-borne borreliosis coincides with tick-borne encephalitis, and the disease is registered throughout the Russian Federation. However, the incidence of Lyme disease is 2-4 times higher than tick-borne encephalitis, and it occupies one of the first places among natural focal zoonoses. Tick-borne borreliosis is widespread in Europe, Asia, and America. In Russia, borreliosis is widespread in the forest and forest-steppe zones from Kaliningrad to Sakhalin. In European Russia, borreliosis is the most common tick-borne infection.
The risk of getting borreliosis after a tick bite is much higher than tick-borne encephalitis. Natural foci of tick-borne borreliosis coincide with the range of ixodid ticks. The incidence of borreliosis is seasonal and coincides with the activity of ticks. The first patients with tick bites are usually registered in March-April. The latter, in the presence of warm weather, are recorded even in October. Peak activity occurs in May-June. The percentage of ticks infected with borreliosis differs in different regions. A tick can simultaneously be infected with Borrelia, tick-borne encephalitis virus and other pathogens. Therefore, the development of a mixed infection is possible.
Transmission of the infection occurs transmissibly through a tick bite (inoculation), although the possibility of infection cannot be ruled out when tick feces come into contact with the skin, followed by rubbing them in when scratching (contamination). In case of a tick rupture, due to improper removal? the pathogen may enter the wound. The nutritional route of infection through consumption of raw goat or cow milk is discussed.
The main risk groups are workers of forestry farms, timber industry enterprises, hunters, foresters and residents of forested areas.
The carriers of Borrelia are ticks of the genus Ixodes, in our country and Europe - I. ricinus and I. persulcatus, in America - I. pacificus and I. scapularis. The life cycle of these ticks (larva - nymph - adult) lasts an average of three years. Ticks become infected from numerous rodents, as well as hares, hedgehogs, birds, etc. Ticks live in grasses, ferns and low shrubs.
Lyme disease (Tick-borne borreliosis, Lymeborreliosis)
Stage of local infection
After the end of the incubation period (about 7-14 days), the stage of local infection begins, characterized by skin manifestations and intoxication syndrome. At the site of the tick bite, an itchy, slightly painful red papule appears, prone to peripheral growth (tick-borne erythema migrans). As the area of redness expands, erythema migrans takes the form of a ring with a diameter of 10-20 cm, having a bright red rim along the edges and a paler central part. In most cases, erythema migrans in Lyme disease resolves spontaneously within 1-2 months, leaving behind mild pigmentation and scaling. Local manifestations of Lyme disease are accompanied by a general infectious syndrome: fever with chills, headache, arthralgia, pain in bones and muscles, and severe weakness. Other symptoms in stage I may include urticaria, conjunctivitis, regional lymphadenitis, runny nose, and pharyngitis.
Dissemination stage
Over the next 3-5 months, the disseminated stage of Lyme disease develops. In an erythematous form of infection, tick-borne borreliosis can immediately manifest with systemic manifestations. Most often, damage to the nervous and cardiovascular systems develops at this stage. Among the neurological syndromes for Lyme disease, the most typical are serous meningitis, encephalitis, peripheral radiculoneuritis, neuritis of the facial nerve, myelitis, cerebral ataxia, etc. During this period, manifestations of Lyme disease may include throbbing headache, photophobia, myalgia, neuralgia, significant fatigue, sleep disorders and memory, disorders of skin sensitivity and hearing, lacrimation, peripheral paralysis and paresis, etc.
Cardiac syndrome in Lyme disease in most cases is represented by atrioventricular blockades of varying degrees, rhythm disturbances, myocarditis, pericarditis, and dilated cardiomyopathy. Joint damage is characterized by migrating myalgia and arthralgia, bursitis, tendonitis, and arthritis (usually in the form of monoarthritis of a large joint, less often - symmetrical polyarthritis). In addition, the course of the disseminated stage of Lyme disease may include damage to the skin (multiple migratory erythema, lymphocytoma), genitourinary system (proteinuria, microhematuria, orchitis), eyes (conjunctivitis, iritis, chorioretinitis), respiratory tract (angina, bronchitis), digestive system (hepatitis, hepatolienal syndrome), etc.
Persistence stage
Lyme disease becomes chronic 6 months to 2 years after the acute stage. In the late stage of Lyme disease, skin lesions most often occur in the form of atrophic acrodermatitis or benign lymphoplasia or joint damage (chronic arthritis). Atrophic acrodermatitis is characterized by the appearance of swollen, erythematous lesions on the skin of the extremities, in place of which atrophic changes develop over time. The skin becomes thin, wrinkled, and telangiectasia and scleroderma-like changes appear on it. Benign lymphocytoma has the appearance of a reddish-cyanotic node or plaque with rounded outlines. Usually localized on the skin of the face, ears, axillary or groin area; in rare cases, it can transform into malignant lymphoma.
Chronic Lyme arthritis is characterized not only by damage to the synovial membrane of the joints, but also to periarticular tissues, leading to the development of bursitis, tendonitis, ligamentitis, and enthesopathies. In terms of its clinical course, arthritis in the late stage of Lyme disease resembles rheumatoid arthritis, Reiter's disease, ankylosing spondylitis, etc. In the late stages of chronic arthritis, thinning of the cartilage, osteoporosis, and marginal abnormalities are revealed by X-ray.
In addition to skin and joint syndromes, at the chronic stage of Lyme disease, neurological syndromes can develop: encephalopathy, chronic encephalomyelitis, polyneuropathy, ataxia, chronic fatigue syndrome, dementia. With transplacental infection, pregnancy can result in intrauterine fetal death and miscarriage. In live-born children, intrauterine infection leads to prematurity, causes the formation of congenital heart defects (aortic stenosis, aortic coarctation, endocardial fibroelastosis), and delayed psychomotor development.
Pathogenesis
Clinical symptoms that appear at different stages of the disease are caused by a combination of immunopathological reactions and the presence of the pathogen and its antigens in the tissues. Penetrating into the human body, borrelia at the site of introduction cause the formation of a primary affect - papules, tick-borne erythema, then hematogenously enter various organs and tissues, where they are adsorbed on cells, interacting most actively with galactocerebrosides of neuroglial membranes. Perivascular infiltrates appear, consisting of lymphocytes, macrophages, plasma cells, and diffuse infiltration of damaged tissues by these elements. Borrelia and the resulting immune complexes lead to the development of vasculitis and vascular occlusion. Borrelia are capable of persisting in tissues for a long time, up to several years, especially in the absence of treatment, which is associated with a chronic relapsing course of the disease.
In the later stages of the disease, borrelia, playing the role of a trigger, provoke the development of immunopathological processes that are of great importance for the pathogenesis of neuroborreliosis and chronic arthritis. Among this kind of patients, the most common are those with the HLA-DR2 and HLA-DR4 genotypes. Already in the early stages of the disease, specific antibodies are produced, the titer of which increases over the course of the disease. The immune response is most pronounced in the later stages, especially when joints are affected. With effective therapy and recovery, antibody levels normalize. Their long-term persistence or appearance in high titers in later stages indicates the persistence of the pathogen even in the absence of clinical manifestations.
Disease or syndrome?
Not only doctors argue about the problem of tick-borne borreliosis; there is no unity among scientists either.
According to one point of view, standard antibiotic therapy cannot destroy all pathogens in the body of patients with weak immune systems. This opinion is confirmed by experiments on laboratory animals: live Borrelia were found after treatment with antibiotics in the body of infected laboratory mice and monkeys. The results of some studies suggest that Borrelia colonies may continue to live in organs and tissues as part of so-called biofilms
— communities of microorganisms enclosed in the polymer matrix they produce. In this form, Borrelia become practically inaccessible to drugs and cells of the immune system.
Borrelia enter the human body along with the saliva of the tick. When a tick begins feeding, it can transmit bacteria only if it is already in the salivary glands, which is the case for about a third of hungry ticks. If they are in the intestines of the tick, then infection can only occur on the second or third day after the tick has been sucked on. Borrelia can also be transmitted through tick feces or when it is crushed if they get into microcracks in the skin or on the conjunctiva of the eyes. Transmission of the pathogen through dairy products that have not undergone heat treatment and infection of the fetus due to borreliosis infection of the mother are also possible. Up
- the front, cone-shaped protrusion of the tick’s body, called the “head” (view from the ventral side). Photo by E. Mitrofanova (IVEP SB RAS, Barnaul)
According to another point of view, after a course of antibiotic therapy there are no living Borrelia left in the body. However, during the course of illness, bacteria manage to cause disturbances in the functioning of the immune system, which manifest themselves for a long time in the form of autoimmune lesions. Strong immunogens are, for example, peptidoglycans
the cell wall of bacteria that can survive in the body for a long time.
Long-term toxic effects can also be caused by the remains of biofilms with dead Borrelia. All these bacterial components provoke inflammatory processes affecting various organs and tissues, which leads, for example, to arthritis. This painful condition was called post-Lyme syndrome
(Blaut-Jurkowska, Jurkowski, 2016).
By the way, a number of experts believe that chronic Lyme disease develops when the patient is simultaneously affected by Borrelia and other pathogens carried by ticks (for example, Rickettsia
). Ticks very often carry pathogens of different infections at the same time, and some of them cause symptoms that are clinically difficult to distinguish.
In the early stages of tick-borne borreliosis, people may experience a wide variety of cold-like symptoms: fever, fatigue, sleep disturbances, and swollen lymph nodes.
In the future, if left untreated, the joints, especially the knees, may become swollen and painful. Neurological problems arise (encephalitis, meningitis, temporary paralysis of the facial muscles), as well as muscle dysfunction, myositis. In later stages of the disease, symptoms vary greatly. Some patients experience heart rhythm disturbances, inflammation of the eyes and liver, and severe weakness. Neurological complications include severe depression, memory impairment, insomnia, frequent headaches, intolerance to light or sounds, hallucinations, encephalomyelitis, etc.
Borreliosis infection
The incubation period ranges from 2 to 30 days, with an average of 14 days. The infection may be asymptomatic, but may also have a different clinical picture of the disease. The infection is divided into three stages, but in principle these are different clinical pictures of the disease. The division of the disease into stages is arbitrary, and clinical manifestations of all stages of the disease in one patient are not necessary. In some cases, the first stage may be absent, in others - the second or third. Sometimes the disease manifests itself only in the chronic stage, so the general practitioner should remember that patients with arthritis, polyneuropathy, encephalomyelitis and other syndromes characteristic of Lyme disease must be examined to exclude borreliosis.
Stage 1: Early local infection
It is characterized by the development at the site of introduction of the pathogen of a primary affect in the form of chronic migratory erythema of Afzelius-Lipschütz, which is a single (sometimes several) rounded red spot at the site of the bite, which over the course of several weeks, gradually growing centrifugally, reaches 15-20 cm or more in diameter .
As the erythema grows, its central part undergoes regression; in its area a mark (in the form of a reddish dot) from a tick bite can be clearly visible. Most often the lesion is localized on the torso, limbs, but can also be on the face. As it grows, the marginal border of the erythema can rupture, turning into a garland-like strip that sometimes passes through the chest, neck, and face of the patient. Erythema at the site of a tick bite is the main clinical sign of Lyme disease. Erythema is usually hot to the touch, painful, often accompanied by itching and burning, its shape is round or oval, less often - irregular. Erythema can persist for a long time (months), sometimes disappears without treatment after 2-3 weeks, in some cases faster (after 2-3 days). Against the background of etiotropic therapy, it quickly regresses and by the 7-10th day it completely disappears, without a trace or leaving behind pigmentation and peeling.
A crust or scar remains at the site of the tick bite. In a number of patients, “daughter” erythema occurs not only at the site of the tick bite, but also on other areas of the skin, due to the hematogenous spread of Borrelia. Compared to the primary lesion, they are smaller in size and do not have traces of a tick bite and an induration zone in the center. Erythema can occur without fever and without intoxication, being the only symptom of Lyme disease, but in 30-60% of cases it may be absent. Patients often experience an intoxication syndrome: headache, chills, nausea, fever from low-grade to 40˚C, myalgia and arthralgia, severe weakness, fatigue, drowsiness. Regional lymphadenitis and stiffness of the neck muscles are often detected at the site of the tick bite. Of the general toxic symptoms, the most constant are weakness and drowsiness. At the 1st stage of the disease, antibodies to Borrelia may often not be detected, but their study is necessary to prevent later complications of the disease.
Stage 2. Early disseminated borreliosis
Stage 2 of the disease, caused by lymphogenous and hematogenous dissemination of the pathogen and developing from the 2nd to the 21st week of the disease (usually in the 4-5th week), is characterized by lesions of the nervous system (serous meningitis, neuritis of the cranial nerves, radiculoneuritis) , cardiovascular system (myocarditis, pericarditis, conduction disorders (especially atrioventricular block). A flu-like syndrome often occurs (headache, fever, weakness, myalgia). Skin lesions at this stage may have the character of secondary ring-shaped elements with a diameter of 1-5 cm, erythematous rash on the palms of the type of capillaritis, urticarial rashes, as well as benign lymphocytoma of the skin of Spiegler.
Mild symptoms of meningeal irritation may appear early, when erythema still persists, and pronounced neurological symptoms are more often observed several weeks after the onset of the disease, when erythema - a marker of tick-borne borreliosis - has already disappeared. Serous meningitis is accompanied by headache of varying intensity, nausea, vomiting, photophobia, soreness of the eyeballs, stiff neck, and other symptoms of irritation of the meninges are less common.
In 1/3 of patients, moderate symptoms of encephalitis are found in the form of sleep disturbances, decreased attention, memory disorders, increased excitability, emotional disorders, etc. Neuritis of the cranial nerves occurs in more than half of the patients. The VII pair of cranial nerves is most often affected, often with paresis of the facial muscles, numbness and tingling of the affected half of the face, pain in the ear or lower jaw, without clear disturbances of sensitivity. The oculomotor, visual, auditory, and rarely the IX-X pairs of cranial nerves may also be affected. Damage to peripheral nerves is also observed. Radicular sensitivity disorders occur in the cervical, thoracic, and lumbar spine. One of the typical neurological disorders is Bannwart syndrome, which includes serous meningitis and damage to the spinal nerve roots with a predominant localization in the cervicothoracic spine.
Neurological disorders usually disappear completely after 1 month, but can recur and become chronic. Damage to the nervous system may be the only manifestation of Lyme disease when general infectious syndrome and erythema are absent. In the 5th week, approximately 8% of patients experience cardiac disorders: pain, discomfort in the heart area, interruptions in heart contractions. The ECG shows atrioventricular block of varying degrees and diffuse damage to the heart muscle. Myocarditis and pericarditis may develop. The duration of cardiac symptoms ranges from several days to 6 weeks. Throughout the entire period, weakness and migrating pain in the bones, muscles, and joints persist.
Stage 3. Late chronic borreliosis
Stage 3 of the disease is characterized by joint damage. It begins 2 months or later from the onset of the disease, sometimes after 1-2 years. Large joints are usually affected, especially the knees, often with unilateral localization. In some cases, symmetrical polyarthritis develops. Arthritis, as a rule, recurs over several years and becomes chronic with destruction of bones and cartilage. At a late stage of the disease, persistence of the pathogen in the patient’s body leads to a chronic course of the disease.
Chronic Lyme disease occurs with alternating remissions and relapses, sometimes becoming continuously relapsing. The most common syndrome is arthritis. Changes typical of chronic inflammation develop: osteoporosis, thinning and loss of cartilage, and less commonly, degenerative changes. Often there is a skin lesion in the form of benign lymphocytoma, which is a dense, edematous, bright crimson infiltrate (or nodule), slightly painful on palpation, located on the earlobe or around the nipple of the mammary gland and lasting from several days to months and even years .
Another lesion typical of the late stage is chronic atrophic acrodermatitis: cyanotic-red spots on the extensor surfaces of the extremities, tending to peripheral growth, fusion, and periodic inflammation. Gradually, the skin at the site of the spots atrophies and takes on the appearance of tissue paper. The process develops over several months and years. The neurological manifestations of chronic Lyme disease, neuroborreliosis, consist of progressive chronic encephalomyelitis and polyneuropathies. Encephalomyelitis is similar to multiple sclerosis. Mental disorders are observed - memory, sleep, speech disorders. Polyneuropathies are accompanied by impaired sensitivity, distal paresthesia, radicular pain, etc. The protracted and chronic course of the disease sometimes leads to partial or complete loss of ability to work.
Lyme disease, or tick-borne borreliosis
Encephalitis
Arthritis
Vomit
Borreliosis
Tick bite
21232 November 22
IMPORTANT!
The information in this section cannot be used for self-diagnosis and self-treatment.
In case of pain or other exacerbation of the disease, diagnostic tests should be prescribed only by the attending physician. To make a diagnosis and properly prescribe treatment, you should contact your doctor. Lyme disease: causes, symptoms, diagnosis and treatment methods.
Definition
Lyme disease is an infectious transmissible natural focal disease caused by spirochetes and transmitted by ixodid ticks, which tends to be chronic and relapsing and primarily affects the skin, nervous system, musculoskeletal system and heart.
Causes of Lyme disease
Lyme disease is caused by gram-negative spirochetes of the genus Borrelia burgdorferi
. Ixodid ticks carry the infection, most often they stick to the neck, chest, armpits, groin folds, i.e. in places with thin skin and abundant blood supply. In children, a relatively common place for ticks to attach is the scalp.
From the moment a tick lands on a person’s clothing until it is sucked on, it takes approximately 1-2 hours.
The causative agent of Lyme disease enters the body with the tick's saliva. Migrating ring-shaped erythema develops on the skin at the site of tick suction. From the site of introduction, the pathogen enters the internal organs, joints, lymph nodes and meninges through the lymph and blood flow. When Borrelia die, they release endotoxin, which causes a cascade of immunopathological reactions.
Several other routes of transmission of Borrelia have been described:
- nutritional route - when eating goat's milk that has not undergone heat treatment;
- intrauterine infection (from mother to fetus), accompanied by congenital anomalies of fetal development, miscarriages and fetal death - especially when infected in the early period of pregnancy. Human susceptibility to Borrelia is high, if not absolute. Stable immunity is not formed - those who have recovered from the disease can become infected many times.
Classification of the disease
Lyme disease can occur in acute, subacute and chronic forms.
There are erythemal (with skin lesions) and non-erythemal forms with predominant damage to the nervous system, heart, and joints.
According to the severity, borreliosis is classified into severe, moderate and mild.
Symptoms of Lyme disease
Acute and subacute course
The incubation period ranges from 3 to 30 days, with an average of two weeks. The onset of the disease, as a rule, has the characteristic features of an infectious process and often occurs with skin lesions. One of the first symptoms is erythema migrans around the place where the ixodid tick has attached itself, and intoxication. In the non-erythema form of borreliosis, the leading symptom is intoxication (headache, chills, nausea, migrating pain in bones and muscles, arthralgia, general weakness, fatigue, low-grade fever up to 40°C).
The febrile period can last several days (usually no more than 15 days). In most cases, the general intoxication syndrome is moderately expressed.
At the site of tick attachment at the end of the incubation period, patients note slight itching, sometimes pain, redness of the skin (erythema) with slight infiltration of the subcutaneous tissue. The erythema gradually increases, reaching a size of 5-15 cm, rarely up to 50 cm or more. The spot has a round or oval shape with a strongly hyperemic outer edge that rises above the level of the surrounding skin. After a few days, the central part of the erythema turns pale or acquires a bluish tint.
In some patients, foci of skin inflammation appear not only at the site of tick suction, but also in other parts of the body, which is explained by the spread of borrelia from the primary focus through the blood and lymph flow. Without treatment, erythema persists for 3-4 weeks (rarely several months) and then disappears. In its place, peeling of the skin, pigmentation, itching, tingling sensation, and decreased sensitivity may be observed.
Atypical variants of erythema migrans are common:
- spot diameter less than 5 cm;
- erythema has the shape of a strip or semiring;
- the central part of the erythema is covered with scales, vesicles, erosions, hemorrhagic rashes, especially when localized on the back surface of the legs.
Lyme disease, which occurs without skin lesions, is characterized by the development of pathological signs from internal organs (nervous system, joints, heart, eyes, etc.) 2-10 weeks after the onset of the disease.
Most often, damage to the nervous system is observed: meningitis (meningoencephalitis), neuritis of the cranial nerves, radiculoneuritis. With meningitis, patients experience headaches of varying intensity (from mild to unbearable), photophobia, increased sensitivity to sound and light stimuli, pain when moving the eyeballs, they are tormented by nausea and vomiting, and moderate rigidity (stiffness) of the neck muscles is detected. Neuritis of the cranial nerves occurs in approximately half of patients with neurological disorders and is manifested by dysfunction of the facial muscles, numbness and tingling of the affected half of the face.
Pain in the ear and lower jaw indicates involvement of the V pair of cranial nerves in the pathological process. The oculomotor, optic, auditory nerves, and, less commonly, the glossopharyngeal and vagus nerves may also be affected. Neurological symptoms with proper treatment usually disappear after a few months, although they may recur, which indicates chronicity of the disease.
Heart lesions usually appear 5-6 weeks after the onset of the disease. Patients complain of discomfort and pain in the heart area, rapid heartbeat, shortness of breath, and dizziness.
Arthritis usually develops 4-6 weeks after the onset of the disease or after erythema migrans, which is observed in approximately 40% of patients with lesions of the musculoskeletal system.
In Lyme disease, arthritis affects large joints: knees, shoulders, elbows and ankles.
Chronic course
The course of the disease is regarded as chronic when the clinical manifestations of Lyme disease persist for more than 6 months. In this case, a progressive chronic inflammatory process develops on the skin, joints or nervous system, and less often in other organs.
Damage to the central nervous system is indicated by long-lasting headaches, fatigue, memory loss, sleep disturbance, which fits into the clinic of astheno-vegetative syndrome.
Encephalopathy is considered one of the manifestations of the chronic course of Lyme disease.
Damage to the peripheral nervous system usually affects the cervical, thoracic and lumbar spine. Patients complain of pain or distal parasthesia in the extremities, sometimes accompanied by moderate muscle weakness. Patients may have symptoms of sensory impairment such as socks and gloves, both symmetrical and unilateral.
In approximately 10-15% of patients with symptoms of acute arthritis, the disease becomes chronic. Arthritis in chronic borreliosis usually affects one or two large joints (most often the knees). Often, in the presence of a leading articular syndrome in the clinic of borreliosis, the lesions spread to the cardiovascular system and skin in the form of various dermatitis.
Diagnosis of Lyme disease
Diagnostic measures for suspected Lyme disease include laboratory and instrumental examination methods.
Laboratory diagnostics:
- determination of increased levels of IgM antibodies to Borrelia (from the 3-6th week of illness);
Diagnostics
Early diagnosis is based on clinical and epidemiological data. With the classic picture of erythema migrans, the diagnosis is made based on clinical signs; the diagnosis is registered even in the absence of laboratory confirmation and data on a tick bite. In other cases, the diagnosis is confirmed by laboratory methods. Culture, detection of pathogen antigen and histological examination of the skin are not sensitive and specific enough; histological examination is, in addition, invasive. Therefore, the diagnosis is confirmed mainly by serological methods - the detection of specific antibodies to the pathogen in the blood.
PCR testing for the presence of genetic material of the pathogen is ineffective in this case. IgG antibodies can be detected 1-3 weeks after infection; the maximum amount of IgG antibodies is synthesized 1.5-3 months after infection. IgG antibodies are often not detected in the early, localized stage of the disease or with early antimicrobial therapy. IgG antibodies circulate in the blood for a long time (from several months to several years), even after successful antimicrobial therapy and cure of the infection. Immunity against Borrelia is not sterile. People who have been ill may become infected again after a few years. False-positive results of determining IgG antibodies to Borrelia may be due to the presence in the blood of specific antibodies for diseases caused by spirochetes (syphilis, relapsing fever); a low level of IgG antibodies is possible in infectious mononucleosis, hepatitis B, rheumatic diseases (SLE), periodontal diseases, in 5-15% of healthy individuals from the epidemic zone.
In the laboratories of the CityLab Association this study is - 45-20-109 - Antibodies to Borrelia IgG (Lyme disease, borreliosis)
Material for research: blood serum.
Collection of material for research: blood is taken into a vacuum tube without preservatives.
Preparation for the study: no special preparation is required.
The study is carried out using the enzyme immunoassay method (ELISA)
Units of measurement: qualitative result.
Interpretation of results
A positive test result indicates a current or past infection. This can sometimes lead to incorrect assessment of the study results if the clinical picture of the disease is atypical.
A negative test result can occur in the absence of infection, when the study is carried out in the early stages of the disease or in the long term after an infection. It must be remembered that the absence of antibodies does not exclude early infection, but does exclude chronic borreliosis.
If a questionable result is obtained, the test must be repeated after 10-14 days.
In principle, the need for treatment cannot be determined based on serological studies alone and the effectiveness of therapy cannot be assessed. These problems must be resolved individually, taking into account clinical data.
Treatment
Patients with moderate Lyme disease are subject to mandatory hospitalization in an infectious diseases hospital at all stages of the disease. Patients with a mild course of the disease (tick-borne erythema, in the absence of fever and intoxication) can be treated at home. Antibiotics are used as etiotropic drugs, the choice of which, dose and duration of use depend on the stage of the disease, the prevailing clinical syndrome and severity. All those bitten by ticks and who have recovered from Lyme disease are subject to clinical observation for 2 years.
Clinical examination is carried out by an infectious disease specialist or a general practitioner. Patients and persons after a tick bite should be examined clinically and serologically after 3, 6, 12 months and 2 years. According to indications, consultations with a cardiologist, rheumatologist, neurologist are prescribed, an ECG test is performed, a blood test for CRP, rheumatoid factor. Pregnant women bitten by ticks deserve special attention. Due to the lack of specific prophylaxis and the known teratogenic effect of Borrelia in the early stages of pregnancy, it is advisable to decide on an individual basis for maintaining pregnancy.
If late manifestations of borreliosis occur, patients are treated in specialized hospitals (rheumatology, neurology, cardiology) according to clinical indications. Convalescents of borreliosis with residual effects are observed by specialists, depending on the damage to one or another system (neurologist, cardiologist, rheumatologist).
Prevention
There is no prophylactic vaccine to prevent borreliosis. The best prevention is protection against tick bites. Prevention consists of observing individual protection measures against tick attacks and raising awareness among the general public. Proper tick removal is of great importance for preventing infection. If the tick has attached itself, it needs to be removed quickly. Borrelia live in the intestines of the tick and do not immediately enter the bloodstream. The longer the tick was on the body, the higher the risk of borreliosis.
The question of the benefits of preventing borreliosis after a tick bite with antibiotics is controversial. Prescribing antibiotics in the first days after a bite can reduce the risk of illness. But they should only be prescribed by a doctor. If a bite occurs, you should immediately seek medical help.
Due to the lack of specific prevention measures, identifying patients based on early clinical signs and mandatory antibiotic therapy according to a rational regimen are of particular importance to avoid severe late complications.
Used Books
- Ofitserov V.I. Lyme borreliosis and its diagnosis. News "Vector-Best" N 2 (28). June 2003.
- Coyle PK: Neurologic Lyme disease update. 12th International Conference on Lyme Disease and Other Spirochetal and Tick-Borne Disorders, New York, NY, 1999.
- Coyle PK, Schutzer SE, Deng Z., et al: Detection of Bb-specific antigen in antibody-negative cerebrospinal fluid in neurologic Lyme disease. Neurology 45:2010-2015, 1995.
- Coyle PK, Deng Z, Schutzer SE, et al: Detection of Bb antigens in cerebrospinal fluid. Neurology 43:1093-97, 1993.
- Elliott DJ, Eppes SC, Klein JD Teratogen update: Lyme disease. Teratology. 2001
- Fallon BA, Das S, Plutchok JJ, et al: Functional brain imaging and neuropsychological testing in Lyme Disease. Clin Infectious Disease 25(s):57-63, 1997.
- Heertum RV: Functional brain imaging in the diagnosis of chronic CNS Lyme disease. 12th International Conference on Lyme Disease and Other Spirochetal and Tick-Borne Disorders, New York, NY, 1999.
- Jonathan A., Edlow MD, Bull's Eye: Unraveling the Medical Mystery of Lyme Disease, Yale University Press, 2003
- Logigian EL, Johnson KA, Kijewski MF, et al: Reversible cerebral hypoperfusion in Lyme encephalopathy. Neurology 49:1661-1670, 1997.
- Practice Guidelines for the Treatment of Lyme Disease. Infectious Diseases Society of America. Clin Infect Dis. 2006;43:1089-1134
- Prevention of Lyme disease. American Academy of Pediatrics. Committee on Infectious Diseases. Pediatrics. 2000 Jan;105(1 Pt 1):142-7.
- Sood, SK Recommendations for test performance and interpretation from the Second National Conference on Serologic Diagnosis of Lyme disease. Clin Infect Dis. 2002 Jul 19; 35:451-464.
- Steere AC, Coburn J., Glickstein L. The emergence of Lyme disease. J Clin Invest. 2004 Apr 15; 113(8): 1093-1101.
- Tietz Clinical guide to laboratory tests. 4th ed. Ed. Wu ANB- USA, WB Sounders Company, 2006, 1798 p.
- Treatment of Lyme Disease. The Medical Letter, Inc. Volume 47 (Issue 1209) May 23, 2005.
Swords crossed
The problem of chronic borreliosis is especially acute in the United States, where the Infectious Diseases Society of America
, IDSA) until recently generally denied its existence. Only in 2021 was it officially recognized that after treatment for Lyme disease, a number of nonspecific symptoms may persist for a long time in some patients. However, without clinical evidence of the presence of live Borrelia in a patient, IDSA does not recommend attributing such symptoms directly to the previous disease and conducting additional courses of antibiotic therapy. Accordingly, insurance companies refuse to pay for treatment for people suffering from a “non-existent disease.”
Thousands of people in the United States, who have suffered for years from serious illnesses that they associate with the consequences of tick-borne infections, do not agree with this position. Chronic Lyme disease was first noted in the United States 45 years ago: according to some estimates, the number of such patients today reaches 400 thousand people. These people, together with some doctors, organized the International Society for the Control of Lyme Disease and Associated Diseases, which proposes the use of aggressive antibiotic therapy when it is suspected that the observed painful symptoms are caused by a borreliosis infection.
Tick-borne borreliosis has been registered in 73 constituent entities of the Russian Federation. The risk of getting sick is highest in the Kama region, the Urals, the Middle Urals and the south of Western Siberia. Data 1997–2010 From: Medical-geographical atlas of Russia “Natural focal diseases”, 2015, as amended.
Defenders of the official point of view believe that chronic Lyme disease itself was invented by unscrupulous doctors exploiting the desperate condition of patients with an uncertain diagnosis. In their opinion, those patients in whom modern diagnostic methods do not detect Borrelia do not need additional treatment, but the help of a psychiatrist. As a result, people who consider themselves chronically ill are forced to turn to doctors who disagree with the position of the medical authorities and receive treatment at their own expense.
However, most doctors in the USA and Canada follow the instructions of official medicine, which has led to real “Lyme wars”. According to some experts, research into the pathology of Lyme disease has become so politicized that it has made it difficult for American medical journals to publish work on chronic borreliosis and to fund research aimed at studying it.
How to remove it with your hand
The problem of chronic borreliosis in the United States is complicated by the activity of “healers” and “chronic Lyme disease specialists” who artificially stir up fears and make money from patients.
Having intimidated patients experiencing ailments of various natures that are not confirmed by a clear diagnosis, and having convinced them that they have chronic borreliosis, healers prescribe them long-term, expensive treatment according to their own regimens. But many months of antibiotic therapy can be destructive for a weakened body. In addition, by wasting time communicating with charlatans, patients are not treating a real disease, such as Alzheimer's disease. Ultimately, the patient returns to the specialist after spending countless hours on pointless procedures and losing thousands of dollars. In Russia, the situation with chronic borreliosis and complications after this disease is not too different: the same unreliable diagnosis, scientifically unfounded recommendations for the prevention and treatment of borreliosis. Obviously, we also have many patients suffering from chronic infections that were not diagnosed and treated in time. There are also plenty of charlatans offering to cure any disease for a fee. Not to mention representatives of official medicine who are trying to treat diseases such as tick-borne encephalitis with the help of homeopathic remedies, drugs with unproven activity that have not undergone appropriate testing, such as iodantipyrine. Or even dummy drugs that do not contain any active substance at all, such as Anaferon produced by NPF Materia Medica Holding LLC, which is headed by O. I. Epstein, the hero of recent investigations by the Commission for Combating Pseudoscience of the Russian Academy of Sciences.