Compound
| Lyophilisate for the preparation of a concentrate for the preparation of a solution for infusion | 1 fl. |
| active substance: | |
| brentuximab vedotin (a conjugate consisting of a CD30-directed monoclonal antibody (cAC10) covalently linked to monomethyl auristatin E (MMAE) (SGD-1006) | 50 mg* |
| excipients: citric acid monohydrate - 2.1 mg; sodium citrate dihydrate - 56.1 mg; α,α-trehalose dihydrate - 700 mg; polysorbate 80 - 2 mg | |
| *The amount of brentuximab vedotin, including 10% excess, is 55 mg. After reconstitution, each ml of solution contains 5 mg brentuximab vedotin |
Use during pregnancy and breastfeeding
Women of reproductive age should be warned about the need to protect against pregnancy during treatment with brentuximab vedotin and use two methods of effective contraception during the period of use of brentuximab vedotin, as well as for 6 months after the end of treatment. If pregnancy occurs during treatment with brentuximab vedotin, the patient should be informed of the potential hazard to the fetus.
There are no data regarding the use of brentuximab vedotin in pregnant women. The use of the drug during pregnancy is contraindicated.
There are no data regarding the excretion of the drug or its metabolites in breast milk. A risk to the infant cannot be excluded. The use of the drug during breastfeeding is contraindicated.
Male fertility.
It is unknown whether the use of the drug has an effect on human spermatogenesis. Preclinical studies have identified testicular toxicity, which may alter male fertility. The presence of aneugenic effects in MMAE has been established. Men planning treatment with brentuximab vedotin are advised to provide sperm samples before starting therapy. Men undergoing treatment with brentuximab vedotin and for 6 months after the last dose of the drug are advised to use an appropriate method of barrier contraception and are not advised to plan to conceive a child.
Pharmacodynamics
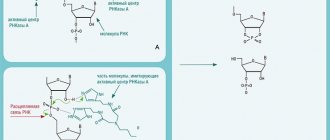
Brentuximab vedotin is a monoclonal antibody-antitumor agent conjugate that is delivered to tumor cells expressing the CD30 antigen and induces their selective apoptosis. In preclinical studies, the biological activity of brentuximab vedotin was found to be the result of a multistep process. The binding of an antibody-antitumor agent conjugate to the CD30 antigen on the cell surface triggers the process of endocytosis, as a result of which the “conjugate-CD30” complex enters the cell and is transported to lysosomes. Inside the cell, the active component monomethyl auristatin E (MMAE) is released through proteolytic cleavage. The binding of MMAE to tubulin leads to the destruction of the microtubule network inside the cell, inhibition of the cell cycle, and ultimately the death of the CD30-expressing tumor cell.
In patients with classical Hodgkin lymphoma and systemic anaplastic large cell lymphoma (ALCL), the CD30 antigen is expressed on the surface of tumor cells. This expression is independent of the stage of the disease, previous therapy and transplantation. Due to its CD30-targeted mechanism of action, brentuximab vedotin has the potential to overcome chemotherapy resistance, as patients refractory to multi-drug chemotherapy consistently express CD30 antigen, regardless of prior transplantation status.
Additional mechanisms of action of antibodies due to their other properties cannot be excluded. The CD30-targeted mechanism of action of brentuximab vedotin, the stable expression of CD30 in patients with classical Hodgkin's lymphoma and systemic ALCL, as well as the therapeutic spectrum of use and clinical evidence of the drug's effectiveness in the treatment of these two CD30-positive tumors, even after several prior lines of therapy, provide a biological rationale use of this drug in patients with relapsed or refractory Hodgkin lymphoma and systemic ALCL with and without prior autologous stem cell transplantation.
Pharmacokinetics
Suction
Cmax of brentuximab vedotin was generally observed at the end of the infusion procedure or at the sampling point closest to the end of the procedure. A multiexponential decrease in serum concentrations of brentuximab vedotin was observed with a terminal T1/2 of approximately 4–6 days. Concentrations were approximately proportional to doses administered. The minimal or no accumulation of brentuximab vedotin observed with multiple doses every 3 weeks is consistent with the estimated duration of terminal T1/2. The typical Cmax and AUC values for brentuximab vedotin after a single dose of 1.8 mg/kg, according to a phase I study, were 31.98 μg/ml and 79.41 μg·day/ml, respectively.
The main metabolite of brentuximab vedotin is MMAE. The median Cmax, AUC, and Tmax for MMAE after a single dose of 1.8 mg/kg in a phase I study were 4.97 ng/mL, 37.03 ng day/mL, and 2.09 days, respectively. MMAE levels decreased after multiple doses of brentuximab vedotin and were approximately 50–80% of the first dose level.
MMAE is then metabolized predominantly to a metabolite exhibiting equivalent activity. However, the exposure of the metabolite is an order of magnitude lower than that of MMAE. Thus, the activity of this metabolite will not have any significant effect on the manifestation of the systemic effects of MMAE.
In the first cycle, increased MMAE levels correlated with an absolute decrease in neutrophil counts.
Distribution
in vitro studies
The binding level of MMAE to human plasma proteins ranged from 68 to 82%.
MMAE is not expected to displace other substances or be displaced by drugs with a high degree of plasma protein binding. In in vitro
, MMAE was a substrate of P-gp and did not inhibit it at clinical concentrations. In humans, the average Vd at Css of the drug conjugate is 6–10 l. Based on population pharmacokinetic analysis, the characteristic apparent Vd (Vd of the VM metabolite or Vd in the peripheral VMP compartment) of MMAE was 7.37 and 36.4 L, respectively.
Metabolism
Brentuximab vedotin is expected to be catabolized as a protein with recycling or excretion of the amino acid component.
In vivo data
studies in animals or humans suggest that only a small fraction of MMAE released from brentuximab vedotin is metabolized.
Levels of MMAE metabolites in human plasma were not measured. At least one MMAE metabolite has shown activity in vitro.
MMAE is a substrate of CYP3A4 and possibly CYP2D6. In vitro data
indicate that MMAE is metabolized predominantly by oxidation via CYP3A4/5.
in vitro
studies using human liver microsomes, MMAE was shown to have an inhibitory effect on CYP3A4/5 only at concentrations well above those acceptable for clinical use. MMAE does not inhibit other isoforms.
MMAE did not activate any of the major CYP450 enzymes in primary cultures of human hepatocytes.
Removal
Brentuximab vedotin is eliminated through catabolism with a typical clearance and T1/2 of 1.457 L/day and 4–6 days, respectively.
Elimination of MMAE was limited by the rate of its release from the monoclonal antibody conjugate, with typical clearance and T1/2 of MMAE being 19.99 L/day and 3–4 days, respectively. A elimination study was conducted in patients receiving brentuximab vedotin at a dose of 1.8 mg/kg. Approximately 24% of total MMAE administered as a monoclonal antibody conjugate during a brentuximab vedotin infusion was detectable in urine and feces over 1 week. Of this amount, approximately 72% was found in feces. A smaller amount of MMAE (28%) was excreted by the kidneys.
Special patient groups
Population pharmacokinetic analysis showed that baseline serum albumin concentrations significantly influence the clearance of MMAE. The analysis showed that in patients with low serum albumin concentrations (<3 g/dL), the clearance of MMAE was 2 times lower compared with patients with normal serum albumin concentrations.
Liver failure.
Studies were conducted on the pharmacokinetics of the drug and MMAE after administration of 1.2 mg/kg of the drug to patients with mild (Child-Pugh class A; n=1), moderate (Child-Pugh class B; n=5) and severe (Child-Pugh class C; n=1) degree of liver failure. Compared with patients with normal liver function, patients with liver failure had an approximately 2.3-fold increase in MMAE excretion.
Kidney failure.
Studies were conducted on the pharmacokinetics of the drug and MMAE after administration of 1.2 mg/kg of the drug to patients with mild (n=4), moderate (n=3) and severe (n=3) renal failure. Compared with patients with normal renal function, MMAE excretion was increased approximately 1.9-fold in patients with severe renal impairment.
Elderly patients.
Clinical studies of brentuximab vedotin did not include a sufficient number of patients over 65 years of age. Therefore, it is currently not possible to determine whether responses to treatment differ between older and younger patients.
Children.
Clinical studies of brentuximab vedotin did not include a sufficient number of patients under 18 years of age. Therefore, it is currently not possible to determine whether pharmacokinetics differ between pediatric and adult patients.
Side effects
Adverse reactions to the drug are ordered by system-organ class and are consistent with the terms of preferred use (in accordance with MedDRA)
(see Table 4). Within the system-organ class category, reactions are distributed according to frequency of occurrence according to the following scheme: very often (≥1/10); often (≥1/100 to <1/10); uncommon (≥1/1000 to <1/100); rare (≥10,000 to <1/1000); very rare (<1/10000); frequency unknown (cannot be calculated from available data).
Table 4
Adverse reactions recorded after using the drug
| Frequency | Adverse reactions |
| Infectious and parasitic diseases | |
| Often | Infection a, upper respiratory tract infection |
| Often | Sepsis/septic shock, herpes zoster, pneumonia, herpes simplex |
| Infrequently | Candidal stomatitis, Pneumocystis pneumonia, staphylococcal bacteremia |
| Frequency unknown | Progressive multifocal leukoencephalopathy |
| From the blood and lymphatic system | |
| Often | Neutropenia |
| Often | Anemia, thrombocytopenia |
| Frequency unknown | Febrile neutropenia |
| From the immune system | |
| Frequency unknown | Anaphylactic reaction |
| Metabolism and nutrition | |
| Often | Hyperglycemia |
| Infrequently | Tumor lysis syndrome |
| From the nervous system | |
| Often | Peripheral sensory neuropathy, peripheral motor neuropathy |
| Often | Dizziness, demyelinating polyneuropathy |
| From the respiratory system, chest organs and mediastinum | |
| Often | Cough, shortness of breath |
| Frequency unknown | Pneumonitis, interstitial lung disease, acute respiratory distress syndrome (ARDS)b |
| From the gastrointestinal tract | |
| Often | Diarrhea, nausea, vomiting, constipation, abdominal pain |
| Infrequently | Acute pancreatitis |
| Frequency unknown | Intestinal obstruction, enterocolitis, neutropenic colitis, erosion, ulcer, perforation and bleedingb |
| From the liver and biliary tract | |
| Often | Increased ALT/AST levels |
| Frequency unknown | Hepatotoxicityb |
| From the skin and subcutaneous tissues | |
| Often | Alopecia, itching |
| Often | Rash |
| Infrequently | Stevens-Johnson syndrome, toxic epidermal necrolysis |
| From the musculoskeletal system and connective tissue | |
| Often | Myalgia, arthralgia |
| Often | Backache |
| General and administration site disorders | |
| Often | Fatigue, chills, fever, infusion reactions in |
| Laboratory and instrumental data | |
| Often | Reducing body weight |
a Preferred usage terms recorded in the Infectious and Parasitic Diseases class include sepsis/septic shock, upper respiratory tract infection, herpes zoster, and pneumonia.
b Some of the listed adverse reactions were fatal.
c Preferred terms associated with the Infusion Reactions class include headache, skin rash, back pain, vomiting, chills, nausea, shortness of breath, itching, and cough.
Selective description of adverse reactions
Neutropenia delayed subsequent infusions in 14% and 22% of patients in phase II and III studies, respectively.
Severe and prolonged (>1 week) neutropenia may occur during treatment with brentuximab vedotin and may increase the risk of severe infections. In phase II studies, the median duration of grade 3 or 4 neutropenia was limited (1 week), with 2% of patients experiencing grade 4 neutropenia lasting >7 days. In less than half of phase II patients, grade 3 or 4 neutropenia was the cause of temporary infection; most patients with associated infections had grade 1 or 2 neutropenia.
In patients participating in phase III studies, grade 3 neutropenia was observed in 22% of patients treated with brentuximab vedotin, and grade 4 neutropenia was observed in 7% of patients in the same group. None of the patients required dose reduction or treatment interruption.
In patients participating in phase III studies, serious infections were observed in 9% of patients treated with brentuximab vedotin. However, there were no cases of bacteremia, sepsis or septic shock in this group. Peripheral sensory neuropathy delayed the next infusion in 13% and 16% of patients in phase II and III studies, respectively. Additionally, peripheral motor neuropathy and upper respiratory tract infection delayed the next infusion in 6% of patients in the phase III study.
Peripheral sensory neuropathy led to dose reductions in 9% and 22% of patients in phase II and III studies, respectively. Additionally, peripheral motor neuropathy also led to dose reduction in 6% of patients in the phase III study. 90 and 68% of patients in phase II and III studies, respectively, continued to receive the recommended dose of 1.8 mg/kg.
In phase II studies of patients with peripheral neuropathy, the mean follow-up from end of treatment to final assessment was approximately 48.9 weeks. At the time of last evaluation, 83% of 89 patients with peripheral neuropathy had resolution or improvement of peripheral neuropathy symptoms. The median duration from onset to resolution or relief of symptoms for all adverse reactions was 16 weeks (range 0.3–106.6 weeks).
Among phase III study patients who developed peripheral neuropathy, the median follow-up from end of treatment to final assessment was approximately 98 weeks. At the last evaluation, 85% of patients who reported developing peripheral neuropathy in the brentuximab vedotin group had resolution or improvement of their peripheral neuropathy symptoms. Overall, the median time to resolution or improvement of peripheral neuropathy in the brentuximab vedotin group was 23.4 weeks (range 0.1 to 138.3 weeks). Infusion reactions were reported in 11% and 15% of patients in phase II and III studies, respectively. In both phase II and phase III studies, adverse events most commonly associated with infusion reactions were mild or moderate in severity (grade 1 or 2). These included headache, skin rash, back pain, vomiting, chills, nausea, shortness of breath, itchy skin and cough.
Cases of anaphylaxis have been reported (see "Special Instructions").
Symptoms of anaphylaxis may include, but are not limited to: urticaria, angioedema, hypotension, and bronchospasm.
Cases of febrile neutropenia have been reported (see "Dosage and Administration"). Grade 5 febrile neutropenia was observed in a patient enrolled in a phase I dose-escalation study after a single dose of 3.6 mg/kg brentuximab vedotin.
Immunogenicity
In two phase II studies, antibodies to brentuximab vedotin were measured every 3 weeks in patients with relapsed or refractory Hodgkin lymphoma or systemic ALCL using a sensitive electrochemiluminescence immunoassay. The phase III study also included patients with Hodgkin lymphoma and an increased risk of relapse or progression after autologous stem cell transplantation. Approximately 7% of patients participating in phase II studies and 6% of patients participating in phase III studies were found to have persistent antibodies to brentuximab vedotin (ATA). In 2 patients participating in phase II studies and 2 patients participating in phase III studies, infusion-related adverse reactions were observed that led to treatment discontinuation.
The emergence of antibodies to brentuximab vedotin did not correlate with a clinically significant decrease in serum levels of brentuximab vedotin, and did not lead to a decrease in the effectiveness of brentuximab vedotin. The appearance of antibodies to brentuximab vedotin did not necessarily lead to the development of infusion reactions. The incidence of infusion reactions was higher in the group of persistently ATA-positive patients (30%), compared with the group of transiently ATA-positive patients (12%) and the group of patients in whom ATA was never detected (7%).
Repeated treatment
Retreatment with brentuximab vedotin was administered to 21 patients with relapsed or refractory Hodgkin lymphoma and 8 patients with recurrent systemic ALCL.
The average number of courses was 7 (range 2 to 37 courses). The types and severity of adverse reactions were consistent with those observed in the phase II combination studies, with the exception of peripheral motor neuropathy, the incidence of which was higher (28% compared to 9% in phase II studies), more often grade 1 or 2. Patients were also more likely to have arthralgia, grade 3 anemia, and back pain compared to patients in phase II studies.
The patient should be informed of the need to inform the doctor about all cases of adverse reactions, incl. not listed in this description.
Interaction
Interaction with drugs metabolized with the participation of CYP3A4 (CYP3A4 inhibitors/inducers)
Coadministration of brentuximab vedotin and ketoconazole, a strong CYP3A4 and P-gp inhibitor, resulted in an approximately 73% increase in concentrations of the antimicrotubulin agent MMAE, with no change in brentuximab vedotin plasma levels. Thus, the use of brentuximab vedotin together with strong inhibitors of CYP3A4 and P-gp may lead to an increased incidence of neutropenia. In case of development of neutropenia, see table. 2 (Dosing recommendations for neutropenia, “Dosage and administration”).
Co-administration of brentuximab vedotin and rifampicin, a strong CYP3A4 inducer, did not change plasma levels of brentuximab vedotin. Although pharmacokinetic data are limited, coadministration of rifampicin appears to reduce plasma concentrations of detectable MMAE metabolites.
The combined use of midazolam, which is a CYP3A4 substrate, and brentuximab vedotin did not alter the metabolism of midazolam. Therefore, brentuximab vedotin is not expected to alter the concentrations of drugs metabolized by CYP3A4 enzymes.
Indications of the drug Adcetris®
treatment of patients with relapsed/refractory CD30+ Hodgkin lymphoma after autologous stem cell transplantation or after at least two lines of prior therapy, when autologous stem cell transplantation or combination chemotherapy are not considered as a treatment option;
treatment of patients with CD30+ Hodgkin lymphoma at increased risk of disease relapse or progression* after autologous stem cell transplantation;
treatment of patients with relapsed/refractory systemic anaplastic large cell lymphoma.
*Factors of increased risk of relapse or progression of the disease are: Hodgkin lymphoma, resistant to first-line therapy; relapse or progression of Hodgkin's lymphoma within 12 months after the end of the first line of therapy; the presence of extranodal lesions, including the spread of nodal masses to vital organs, in case of relapse before autologous hematopoietic stem cell transplantation.